Individuals with diabetes have beta cells that are dead or damaged. These dead or damaged beta cells create insulin. Furthermore, cellular stress is the cause of that production which is created from high levels of metabolic stress. High levels of metabolic stress can be caused by aging and inflammation and other thing health problems.
One element of beta cell failure in type 1 and type 2 diabetes is a flawed stress response. Which is a reaction to chronic, non-stopping stress that compromises the beta cell function. New research from Dhawan and individuals from her lab define novel discoveries about these compromises.
The new research identifies the mechanism by which cellular stress creates cell failure. They discovered an epigenetic regulatory molecule that controls the beta cell stress reaction. Additionally, they uncovered its survival during the period of the beta-cell growth. As well as under the conditions of overnutrition. In doing so, they found this protein also supports beta cell function and survival.

Insulin
In 2019, Fouad R. Kandeel, M.D., Ph.D., director of the Islet Cell Transplantation Program and Arthur D. Riggs, Distinguished Chair in Diabetes & Metabolism Research, opened a trial to learn more about the disease.
They opened a trial to figure out if gastrin, a gut hormone, increases the number of insulin in producing cells. Also to know if they protect beta cells from inflammation damage, could possibly improve the results of islet transplant and reverse type 1 diabetes.
Ten years of research have revealed that an islet cell transplant can help in treating unstable type 1 diabetes. It helps by balancing blood sugar levels. Furthermore, it can even stop the usage of insulin treatment for some individuals. Although, majority of the individuals needed to repeat the transplants from multiple donors to get enough islets. Meaning, they needed multiple donors in order to have independence from their insulin. Also the provided donor islet cells are limited.
Trials
All of the gastrin trial participants had better blood sugar levels at the end of the trials. The individuals did not have to use insulin everyday. More than 50% of the participants stopped using insulin after having one islet transplant.
The patients in the trial received one islet transplant. Which was followed up by a 60 day course of gastrin treatment. Additionally, the Individuals received two injections daily during this treatment.
The participants were under surveillance for one year for possible side effects. They also were monitored for changes in their blood sugar level and insulin requirements. The data was correlated to medical records to regulate who had developed diabetes.
Islet
Individuals who didn’t receive gastrin needed to have an average of two to three islet transplants. These findings predict that gastrin protects and supports the transplanted islets that produces insulin.
Originally, insulin was used as the cure of diabetes, but it was also the most significant treatment for any other type of disease. Without the insulin the individual who had diabetes would have died within a few years. Today, diabetes is not as bad as it would have been 100 years ago.
Written by Markita Thomas
Sources :
CNN – Bad habits of night owls may lead to type 2 diabetes , study says
City of Hope – Diabetes experts present exciting new research at ADA conference
National Institutes of Health – Diabetes treatment in 2025: can scientific advances keep pace with prevalence ?
Sleep Foundation – Chronotypes
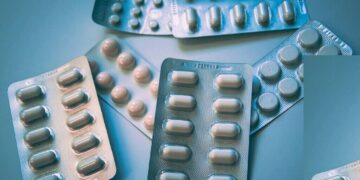
Top and Featured Image Courtesy of SoQ Flickr Page – Creative Commons License
Inset Image Courtesy of Practical Cures Flickr Page – Creative Commons License