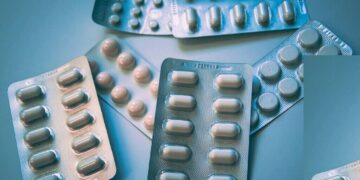
Breast cancer remains one of the most pressing health concerns for women globally, emphasizing the critical importance of effective screening strategies. Recently, there has been considerable debate surrounding the optimal age to commence breast cancer screenings, particularly mammograms, for women. This article aims to explore the latest guidance and recommendations for breast cancer screenings in women aged 40 and older, shedding light on the evolving landscape of preventive healthcare.
The Debate Surrounding Screening Age
For decades, guidelines regarding the initiation of breast cancer screenings have varied among medical organizations, leading to confusion and inconsistency in clinical practice. Traditionally, many organizations, including the American Cancer Society (ACS) and the U.S. Preventive Services Task Force (USPSTF), recommended initiating mammographic screening at age 40. However, in recent years, there has been growing scrutiny over the potential harms associated with early screening, such as false positives, unnecessary biopsies, and overdiagnosis.
Updated Recommendations
In response to mounting evidence and evolving perspectives, several prominent medical bodies have revised their recommendations for breast cancer screenings in women aged 40 and older. The USPSTF, in its latest guidelines published in 2023, now advises biennial mammograms for women aged 50 to 74, with the decision to screen before age 50 left to individual discretion based on risk factors and preferences. Additionally, they recommend discussing the benefits and potential harms of screening with healthcare providers to make informed decisions.
Similarly, the ACS, in its updated guidance released in 2022, suggests that women at average risk of breast cancer should begin annual mammograms at age 45, followed by biennial screenings at age 55 and older. However, they also emphasize the importance of shared decision-making between patients and healthcare providers, considering individual risk factors and preferences.
The decision to initiate breast cancer screenings at age 40 or defer until later hinges on various factors, including personal and familial risk factors, overall health status, and individual preferences. Women with a family history of breast cancer or certain genetic mutations, such as BRCA1 and BRCA2, may benefit from earlier and more frequent screenings due to heightened risk. Conversely, women with significant comorbidities or limited life expectancy may opt for a more conservative approach.

Importance of Shared Decision-Making
Central to the updated guidance on breast cancer screenings is the concept of shared decision-making, wherein patients and healthcare providers collaborate to make informed choices aligned with individual values and preferences. This approach empowers women to actively participate in their healthcare decisions, fostering a sense of ownership and autonomy. Healthcare providers play a pivotal role in facilitating open dialogue, providing evidence-based information, and addressing concerns to support patients in navigating complex screening decisions.
Despite the availability of updated guidelines, disparities persist in access to and utilization of breast cancer screenings, particularly among underserved populations. Socioeconomic factors, including income level, education, insurance coverage, and geographic location, significantly influence screening rates and outcomes. To address these disparities, concerted efforts are needed to enhance access to screening services, promote health literacy, and implement targeted interventions in high-risk communities.
Advancements in Screening Technologies
In addition to revising screening guidelines, ongoing advancements in imaging technologies hold promise for improving the accuracy and efficacy of breast cancer screenings. Digital mammography, 3D mammography (tomosynthesis), and breast magnetic resonance imaging (MRI) offer enhanced sensitivity and specificity, particularly in women with dense breast tissue or elevated risk factors. These innovations underscore the importance of staying abreast of evolving technologies and incorporating them into clinical practice to optimize patient care.
The landscape of the cancer screenings for women aged 40 and older continues to evolve, guided by emerging evidence, shifting perspectives, and advances in technology. Updated recommendations emphasize the importance of shared decision-making, personalized risk assessment, and equitable access to screening services. By empowering women to make informed choices aligned with their values and preferences, healthcare providers can play a pivotal role in reducing the burden of breast cancer and improving outcomes for all.
Written By: Kamaria Morse
Sources:
Rochester First- Mammogram screening age lowered to 40, local doctor weighs in by Taylor Mulligan
Med Page- USPSTF Finalizes New Breast Cancer Screening Recommendations by Mike Bassett
WXZY- Metro Detroit women sound off on new age recommendations for mammograms by Tiarra Braddock
CNN- Task force updates guidance for breast cancer screenings for women 40 and older By Jacqueline Howard
Featured Image Courtesy of Cat Flickr Page – Creative Commons License
Inset Image Courtesy of Maryland GovPics Flickr Page – Creative Commons License