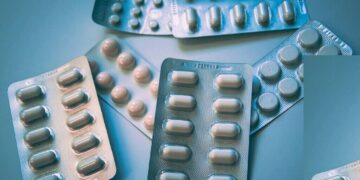
People exhibit similar symptoms when suffering from seasonal allergies or COVID-19. Knowing the differences for the best health outcome is vital, especially in light of recent masking policy changes, new variants, and infection rates creeping back up in the United States.
So, how does a person tell the difference between allergies and coronavirus? Health experts contend the only way to truly know the answer is to take a COVID test and treat any possible symptoms as though it was the virus. Chicago Department of Public Health Commissioner Dr. Allsion Awady advised everyone that they should remain home if they are not feeling well or have tested negative for COVID-19, according to NBC News.
The prominent symptoms of the Omicron variant are cough, congestion, runny nose, and fatigue, explained an infectious disease specialist Dr. Katherine Poehling in January. She noted that not many patients report losing their taste or smell with this variant. It is likely Omicron’s subvariant, BA.2, has similar symptomatology.
Moreover, the Centers for Disease Control and Prevention (CDC) data indicates that some of COVID-19’s most common symptoms overlap with those associated with seasonal allergies; congestion, runny nose, sneezing, and itchy and burning eyes. In addition, children with allergies are typically restless; conversely, adults experience more fatigue.
- If a child is feverish with a persistent cough and listless, with or without a runny nose and itchy eyes, a pediatrician should be notified, reports New York-Presbyterian.
- If a person also has a fever, chills, cough, shortness of breath, muscle or body aches, nausea, vomiting, or diarrhea, they may have COVID.
Emergency warning signs for the virus include problems breathing, continuous pain or pressure in the chest, unusual confusion, inability to awaken or remain awake, and pale, gray, or blue-colored skin, lips, or nail beds, depending on skin tone, according to the CDC. If a person exhibits these symptoms, the CDC recommends they should call 911 or call ahead to the local emergency medical facility: Notify the operator that the caller is seeking care for someone who has or may have COVID-19.

Do Allergies Make People More Susceptible to COVID-19?
There is no evidence that suggests those with pollen-related allergies are more susceptible to coronavirus. However, those with compromised immune systems are at a higher risk of a severe COVID infection.
It is important to note: Seasonal allergy sufferers do not have weakened immunity; their allergies are an overreaction of their immune system, according to William Reisacher, M.D., an associate attending otolaryngologist at NewYork-Presbyterian/Weill Cornell Medical Center.
Having airborne seasonal allergies, pet dander, or food allergies does not disqualify a person from getting a COVID vaccination, even if they receive allergy immunotherapy. However, Dr. Reisacher added that they must speak with their allergist on whether to hold off on being with the treatment around the time they get vaccinated.
COVID vaccinations are available to everyone ages five and older, the first booster can be given to those 12 and older. A second booster can be taken by individuals 50 and older.
Written by Cathy Milne-Ware
Sources:
NBC News Chicago 5: COVID vs. Allergies: Here’s How to Tell the Difference
New York-Presbyterian Health Matters: Is It Seasonal Allergies or COVID-19? By William Reisacher, M.D.
CDC: Allergies and Pollen
Featured and Top Image by Towfiqu Barbhuiya Courtesy of Unsplash – Public Domain License
Inset Image by Kelly Sikkema Courtesy of Unsplash – Public Domain License